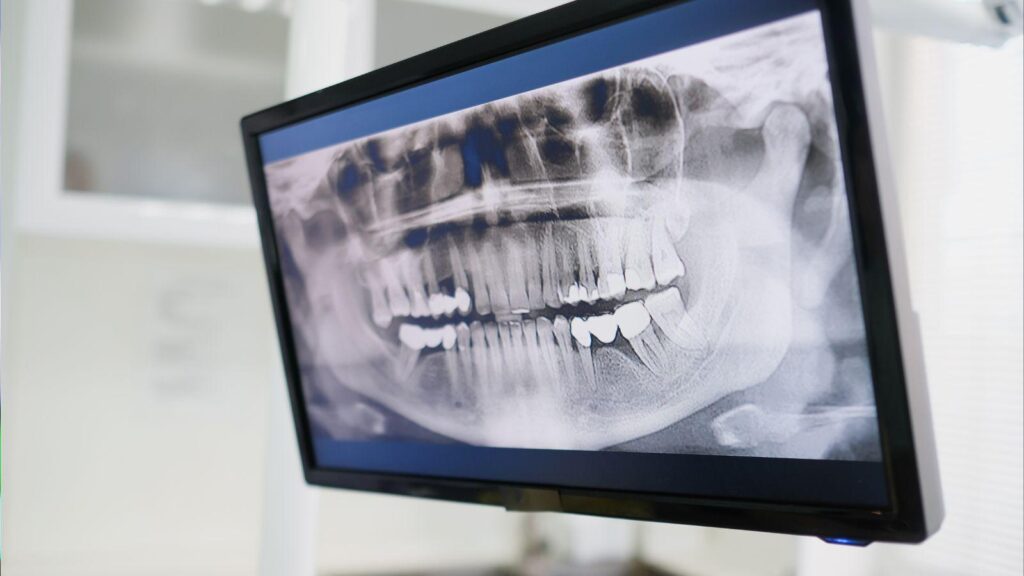
Getting dental implants means planning ahead. You’ll need a combination of dental X-rays and, in many cases, a 3D CT scan so your dentist can check bone quality, nerve positions, sinuses, and where an implant can safely fit — the same thorough imaging process used for a tooth implant in Pittsburgh. These images give the exact information your dentist needs to decide if implants will work for you and to plan the safest, most reliable placement.
As you read on, you’ll learn how each type of image helps assess your jawbone, show nearby nerves and sinuses, and guide precise implant placement. You’ll also see why your medical and dental history matters for a smooth, successful treatment.
Assessing Jawbone Health
You need clear images and measurements to check bone height, width, and quality before an implant. These tests show if you can get an implant now, or if you need bone grafting or other prep first.
Panoramic Radiograph
A panoramic radiograph gives a wide view of your jaws, teeth, and sinuses in one image. It shows overall bone height and major anatomical landmarks, like the mandibular canal and maxillary sinuses, so your dentist can spot large problems or missing bone.
This image uses low radiation and is quick to take. It helps plan whether simple implants are possible and flags areas needing more detailed scans. Panoramic films do not show fine bone detail or exact thickness, so they’re often a first step rather than the only test.
Cone Beam Computed Tomography (CBCT)
CBCT creates 3D images of your jaw, showing bone width, height, and density at the exact implant site. It maps nerve paths and sinus positions, so your surgeon can plan implant angle, length, and avoid nerve or sinus injury.
You receive a higher radiation dose than a panoramic film but still lower than a medical CT. Dentists use CBCT when precise measurements matter—such as narrow ridges, complex anatomy, or when planning bone grafts and guided surgery. Expect short scan time and digital images your team can view from different angles.
Bone Density Evaluation
Bone density affects how well an implant will fuse with your jaw. Dentists assess density using CBCT gray values, clinical probing, and sometimes bone turnover blood tests when needed. Denser bone often supports immediate or early loading; softer bone may need healing time or grafting.
Your clinician may classify bone quality (hard, medium, soft) and choose implant type, surface, and placement technique accordingly. If density is low, options include bone grafts, sinus lifts, or staged implant placement to improve long-term stability.
Evaluating Oral Structures and Implant Placement
You need clear images of bone volume, the sinus spaces above upper teeth, and the path of major nerves. These details guide where implants can go, the size of implants, and whether you need bone grafting or other prep work.
3D Imaging Techniques
You usually get a Cone Beam CT (CBCT) scan for implants. CBCT gives a three‑dimensional view of your jaw, showing bone height, width, and the shape of potential implant sites. Your dentist uses the 3D images to measure bone in millimeters and to plan the exact angle and depth of each implant.
Software can overlay planned implant positions on the scan. That lets your clinician check for proper spacing from adjacent teeth and ensure the final crown will sit correctly. In complex cases, the CBCT file can be used to make a surgical guide that controls drill position during surgery.
Sinus Assessment
If you need implants in the upper back jaw, your dentist examines the maxillary sinuses on the scan. A low sinus floor or large sinus cavity can leave too little bone for an implant. The CBCT shows the sinus membrane, any sinus disease, and areas of reduced bone height.
When bone is insufficient, your dentist may plan a sinus lift or graft. The scan helps decide whether a lateral window or transcrestal lift fits your anatomy best. It also reduces the risk of perforating the sinus membrane during surgery.
Nerve Location Analysis
Finding the inferior alveolar nerve and mental foramen in the lower jaw is critical. The CBCT pinpoints the nerve canal in three dimensions so your dentist can keep a safe distance—usually several millimeters—when choosing implant length and position.
Your clinician also checks for any atypical nerve paths or multiple canals that X-rays might miss. If an implant would come too close to a nerve, options include shorter implants, angled placement, bone grafting, or changing the implant site to avoid nerve injury.
Reviewing Patient Medical History
You must provide a complete, up-to-date medical and dental history before any diagnostic imaging or implant planning. This history guides which scans you need and flags conditions that change treatment timing, implant type, or the need for medical clearance.
Detection of Hidden Oral Issues
Your history helps clinicians target imaging to look for hidden problems that affect implant success. For example, if you report frequent sinus infections, the clinician will order a maxillary sinus-focused CBCT to check for sinus floor anatomy, chronic sinus disease, or sinus septa that could complicate upper implants. If you mention past wisdom-tooth surgery or trauma, scans will check for retained root fragments, bone defects, or altered nerve paths.
Brief dental symptoms you may not notice—like intermittent numbness or a vague ache—also prompt higher-detail imaging. CBCT or periapical radiographs reveal bone loss, periapical infections, and impacted teeth that could undermine an implant if left untreated. Your medication list (bisphosphonates, anticoagulants) and smoking status further influence the decision to image and treat hidden oral disease first.
Identifying Contraindications Through Scans
Your medical history plus targeted scans reveal conditions that may contraindicate immediate implant placement. If you take bisphosphonates or have a history of head-and-neck radiation, CBCT helps assess bone quality and detect osteoradionecrosis risk zones. For patients on blood thinners, imaging defines surgical margins and vascular anatomy to reduce bleeding risk.
Systemic diseases you report—uncontrolled diabetes, autoimmune disorders, or active infections—require imaging to check for poor bone density, cysts, or abscesses that raise implant failure risk. Scans also map the inferior alveolar and mental nerves precisely when you describe numbness or prior nerve injury, avoiding nerve damage during implant placement.